Rocklin, CA
Welcome To Animal Eye Center
Animal Eye Center is a veterinary practice limited to diseases and surgery of the eye. Our board-certified veterinary ophthalmologists are dedicated to providing the most advanced medical and surgical care along with excellent communication with clients and referring veterinarians. Animal Eye Center has been serving the Sacramento and Sierra Nevada Foothill community since 1993.
We Are Passionate About Your Pets Vision And Quality of Life!
About Animal Eye Center
Animal Eye Center is a veterinary hospital whose practice is limited to diseases and surgery of the eye. Our goal is to provide the most advanced medical and surgical care available for our patients. Our surgical facility is one of the few in Northern California equipped to perform Ahmed Gonioimplants and Endolaser Cyclophotocoagulation (ECP) surgeries for the treatment of glaucoma.

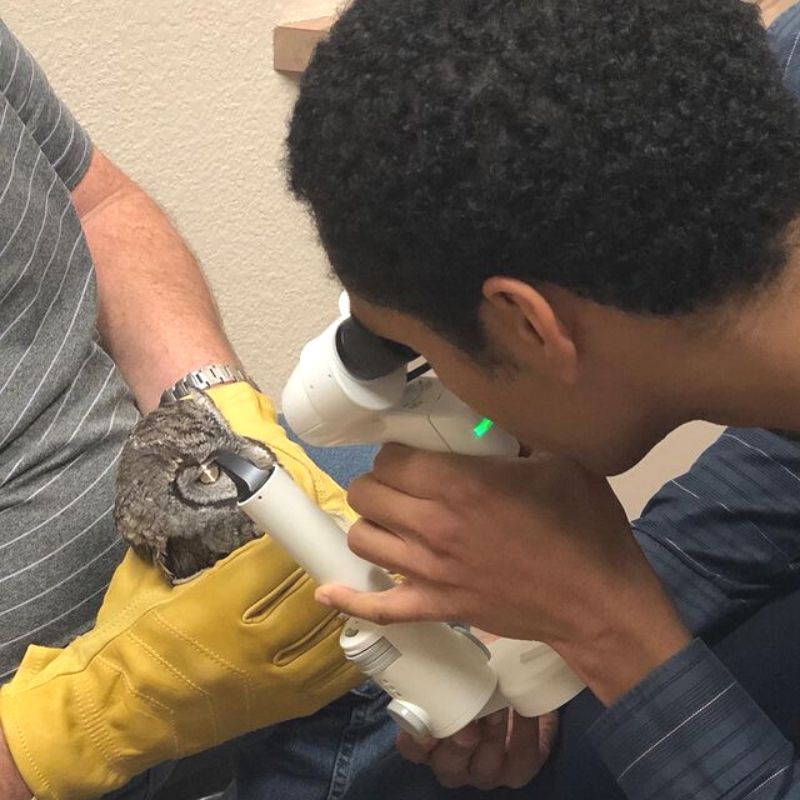

Conditions We Treat
Animal Eye Center offers state-of-the-art medical diagnostics and surgical procedures, including cataract removal by phacoemulsification with intraocular lens implantation. We examine, diagnose, and treat the eyes of all species, including cats, dogs, birds, and other exotic species.

Common Conditions
Eye Problems
- Cataracts
- Glaucoma
- Eye trauma
- Uveitis (eye inflammation)
- Vision loss
- KCS (dry eye)
- Ocular tumors
- Corneal Ulcers and Perforations
- Retinal disease
- Lens luxations
- Eyelid disorders (entropion, distichia)
- Episcleritis/Scleritis
- Congenital Abnormalities
- Feline Herpes Keratitis
- Corneal Dystrophy/ Degeneration
- Several Others

Cataract
What is a cataract?
A cataract refers to an opacity of the lens. The lens is suspended behind the pupil opening in the eye and focuses light onto the retina. The lens opacity or cataract may be small and not affect vision, or it can involve the entire lens resulting in complete blindness. Cataracts can start out as a small opacity and progress to a complete cataract. Animals can be born with cataracts (congenital), or they can develop them secondary to a genetic defect (inherited), old age (senile), or a metabolic defect (diabetic). Some cataracts develop secondary to chronic inflammation in the eye, or they can occur after severe trauma to the eye.

Glaucoma
What is glaucoma?
Glaucoma is increased fluid pressure inside the eye. Normal intraocular pressures (IOP) are below 25 mmHg. When IOP increases over 40 mmHg, severe damage to the retina and optic nerve occurs, and the eye can lose vision within 24 hours. Eyes have a continual production and drainage of fluid or aqueous humor within the eye. Glaucoma occurs as an inherited defect of the drainage angle (primary) where the aqueous humor flows out of the eye or because of an abnormality within the eye (secondary).

Exotic Animals
Exotics Treated
- Birds
- Reptiles
- Amphibians
- Rabbits
- Pocket Pets
- Livestock
- Zoo Animals
- Wildlife
- Fish
Meet Your Pet’s Ophthalmologist
We are a very friendly yet highly professional practice that works with you to achieve the best results for your much-loved pet’s eyes. Our veterinary team genuinely cares for your best friend, and we take pride in taking the time to help you understand your pet’s condition. Our board-certified veterinary ophthalmologists have a vast range of experience and knowledge in small animal and exotic animal eye conditions.
We are supported by a team of trained ophthalmic technicians and support staff to ensure that all our patients receive the best treatment possible.

Dr. Sydney Edwards

Dr. Kristina Gronkiewicz

Our Client Reviews

Dr. Sydney Edwards
Veterinary Ophthalmologist
Dr. Edwards is originally from Charlotte, North Carolina. She received her DVM from North Carolina State University in 2013. Following graduation, she completed a small animal rotating internship at Ohio State University. In 2018, she became board certified after completing a four-year ophthalmology residency at the University of California, Davis.
Dr. Edwards then spent two years in a private ophthalmology practice in Charlotte, NC, before returning to UC Davis for a one-year clinical instructor position. Dr. Edwards joined the ophthalmology team at Animal Eye Center in July 2021 and purchased the practice from Dr. Lana Linton in January 2023. Dr. Edwards’ special interests include ocular surface neoplasia, cataract and glaucoma surgery, and equine ophthalmology.

Dr. Kristina Gronkiewicz
Veterinary Ophthalmologist
Dr. Kristina Gronkiewicz is an Illinois native who received a Doctor of Veterinary Medicine degree from the University of Illinois in 2012, graduating with high honors. Dr. Gronkiewicz then completed a one-year small animal medicine and surgery internship at Oklahoma State University and then a three-year comparative ophthalmology residency and master’s program at the University of Missouri.
Upon completion of the residency program in 2016, Dr. Gronkiewicz became a board-certified veterinary ophthalmologist. In addition to being a diplomate of the American College of Veterinary Ophthalmologists (ACVO), Dr. Gronkiewicz also serves on the ACVO’s public relations committee, helping pet owners understand the importance of veterinary ophthalmologists.
After her residency, Dr. Gronkiewicz left the Midwest and practiced at Animal Eye Center in Rocklin from 2016-2020. Dr. Gronkiewicz then relocated to Seattle and established an ophthalmology department at a multi-specialty private practice, working at the Animal Medical Center of Seattle from 2020-2022.
Dr. Gronkiewicz is looking forward to returning to Animal Eye Center and the Sacramento area. Dr. Gronkiewicz loves all aspects of ophthalmology, but she has a special interest in corneal, glaucoma, and cataract surgeries.

Dr. Christian Munevar
DVM
Dr. Munévar is a California native and graduated from the University of California, Davis School of Veterinary Medicine in 2018, where his interest in veterinary ophthalmology began. He went on to complete a small animal rotating internship at the University of Pennsylvania and did his ophthalmology residency here at Animal Eye Center. He finished his residency in 2022. Dr. Munévar enjoys helping local primary veterinarians with their tough ophthalmology cases and enjoys getting to see a wide breadth of animal patients.



